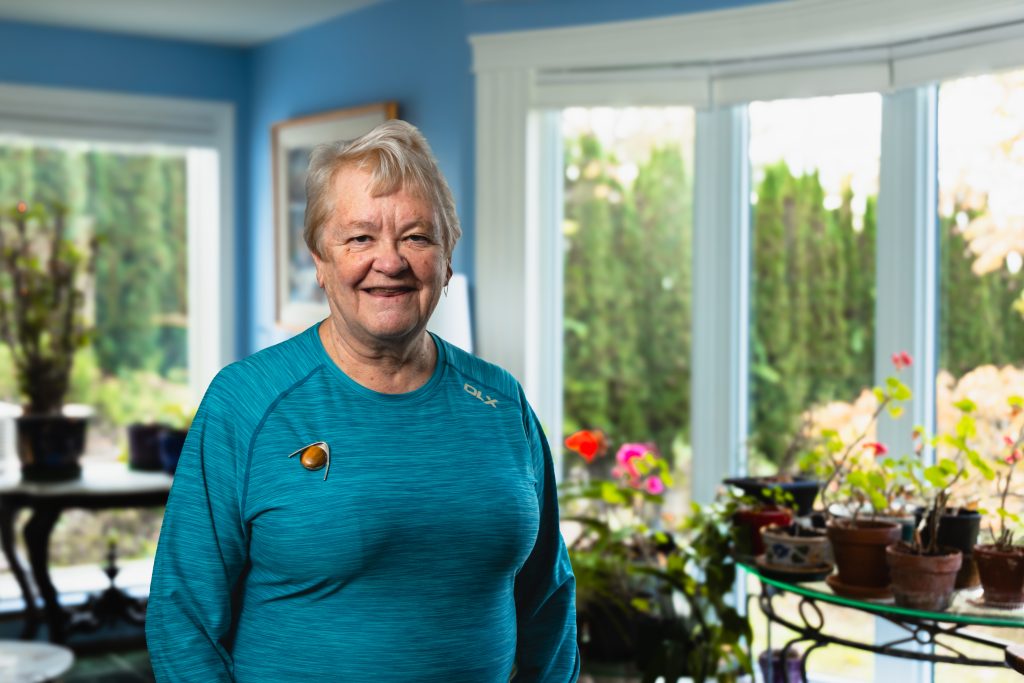News & stories, Forging the future of heart care
May 2023
Donor support drives innovation at the New Brunswick Heart Centre
It was not how Will Thornback expected his day to go. He was working from home in uptown Saint John when, by mid-morning, he felt pain and burning in his chest.
“I thought it was GERD,” he says, using the acronym for gastroesophageal reflux disease. “I just thought I needed an electrolyte drink.”

It was much more serious. Luckily, his wife insisted on calling 911.
Even when EMTs arrived minutes later and told him he was having a heart attack, he was still in disbelief. He had no history of heart disease nor any red-flag risk factors. He was, he thought, a healthy 50-year-old.
But when he was rushed into the Emergency Room at the Saint John Regional Hospital and on to cardiac surgery without delay, the reality – and seriousness – of his condition became undeniable.
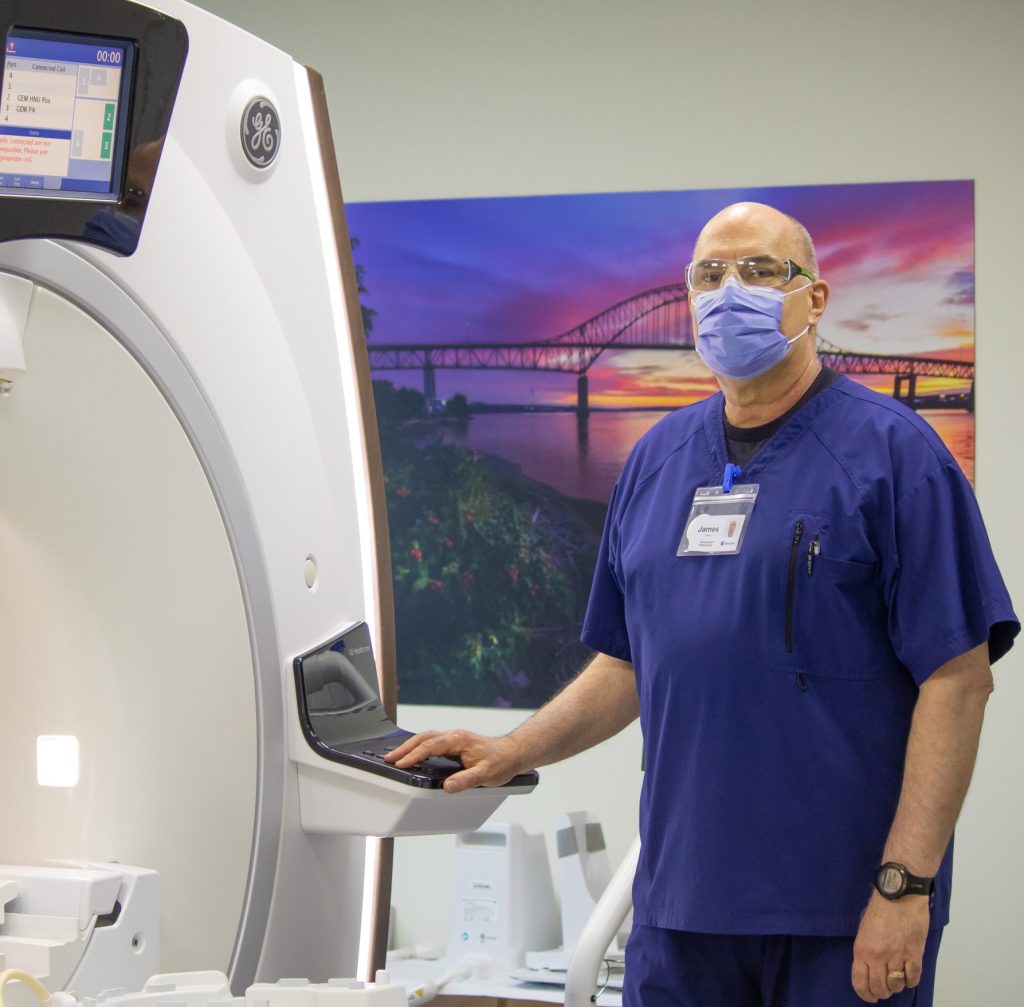
In the New Brunswick Heart Centre’s Cardiac Catheterization Laboratory on the fifth floor of the Saint John Regional Hospital, Mr. Thornback’s surgeon and a team of cardiology nurses went to work on his two blocked arteries. One was completely clogged, the other 80 per cent blocked.
“Everything was happening really quickly,” he says. The heart team moved equipment into place, connected an IV, and got him changed into a hospital gown. Having the head nurse by his side, explaining each step, was a great comfort.
“I wasn’t worried, and I didn’t have any questions because they were telling me everything that was going on,” he says. “They were completely in control. This is something that they do all day long. They’re lifesavers, right?”
Through a small incision in his wrist, his surgeon inserted a small tube – a catheter – with a tiny balloon on the end to stretch the blocked artery. He then placed a stent, a small wire mesh tube that helps keep the artery open.
Laying on the operating table under gentle sedation, Mr. Thornback looked up in awe at a large monitor where an angiogram, a live X-ray of his heart, was displayed.
A computer programmer who co-founded a tech company with his wife, Linda Thornback, he was intrigued by the sophisticated tools surrounding him in the cutting-edge lab. It looked to him like something out of Star Trek.
"I almost forgot that I was having a heart attack; I was so enthralled with the science. From a technology standpoint, it was incredible to witness."
- Will Thornback, patient
Meanwhile, back home, his wife, who could not accompany him to the hospital due to COVID restrictions, waited 30 minutes, as the EMTs had suggested, before checking in with the ER. She was amazed to hear that her husband was already in surgery.
“You realize that those resources are so quickly assembled in an emergency,” she says. “A 100-per-cent blockage can kill you quickly. Will was stented within an hour of us calling an ambulance, and I believe that saved his life.”
Three days later, Mr. Thornback was discharged. Friday afternoon, he was soaking in the warm spring sunshine at Mispec Beach, on Saint John’s East Side, with his family. The shock had worn off, and he was starting to reflect on what he’d gone through.
“Oddly enough, it was a really fantastic experience,” he says.
He marvelled at the winning combination of “science and psychology,” as he puts it, the blend of high-tech tools and human-centred care that made his treatment so timely, compassionate and successful.
Before his heart attack, he had never heard of the New Brunswick Heart Centre. Now, he’s grateful for the quality of care he received there.
“We didn’t know how lucky we were until that day.”
When Dr. Jean-François Légaré came to the New Brunswick Heart Centre in 2016 as Chief of the Division of Cardiac Surgery, he arrived with a vision: “I want this Heart Centre to be the best in Canada.”

"We want to be a model for the future of cardiovascular care."
- Dr. Jean-François Légaré, Interim Medical Director, New Brunswick Heart Centre
Now, as the Centre’s Interim Medical Director, an appointment he received in 2022, Dr. Légaré is leading an ambitious team of physicians, nurses, pharmacists, therapists and other cardiovascular professionals to keep pushing the Heart Centre to the leading edge of cardiac care in this country.
A “big program in a small city,” the Heart Centre has “always punched higher than its weight,” says Dr. Légaré.
Founded in 1991, it provides the full spectrum of cardiac care except for heart transplantation and long-term mechanical support to treat heart failure. (For those services, most patients go to Halifax or Toronto.)
As New Brunswick’s only tertiary cardiac care centre, the Centre serves patients from across the province and much of Prince Edward Island – nearly a million Atlantic Canadians. The only cardiac catheterization, electrophysiology, and cardiac surgical centre in the province, it conducts nearly 1,000 surgeries annually.
“That is in the ballpark of many centres in Canada,” Dr. Légaré says, “and we’re at the cutting edge of what cardiac surgery should look like.”
While technology and tools are part of their evolution, he says one of the Centre’s greatest assets is its team culture.
“There aren’t different silos,” he says. “We all work as a team to approach every single patient.”
That kind of collaboration and support is rare in his highly competitive profession. Having worked at one of the world’s largest cardiac surgery and cardiology centres in Leipzig, Germany, he knows first-hand what that looks like.
“Germany was exciting because it was a very large institution offering world-class care,” he says. “But you were a very small cog in a very large machine.”
He had little patient contact or opportunity to collaborate with his colleagues. He contrasts that with the team at the Heart Centre here, which includes more than 25 physicians from various sub-specialties, a cadre of nurses, pharmacists, therapists, other health care professionals, the administrative team and the cleaning staff.
The Heart Centre is organized to maximize efficiency for patient care and patient visits, which Dr. Légaré says is quite unusual – and beneficial.
“Ultimately, all of this teamwork is very positive for patients,” he says.
That was Mr. Thornback’s experience.
“I’m still amazed at how well they work together, the technology they use, and the team environment between the doctors and the nurses,” he says.
His wife, a project manager, marvels at how integrated and efficient the full spectrum of her husband’s care has been, from the ambulance and emergency surgery to his follow-up at the Heart Centre’s Cardiac Rehabilitation Program, which teaches heart patients healthy habits to manage their disease.
“The way the system is laid out is perfectly designed,” she says. “You can almost see the data flow chart with the arrows pointing to your next step: this is where you go through your blood work, this is where you go through rehab, this is what you do now. Every step is really clear.”
While Will Thornback was just minutes from the Saint John Regional Hospital when his cardiac emergency struck, Tom O’Connor was more than 200 kilometres away when his struck last year.
It was one of those gorgeous March days that could make even the most adamant sunseeker appreciate winter: snow sparkling, clouds skittering across a bright blue sky, the winds light, the air crisp.
Mr. O’Connor, a retired education consultant, saw the perfect conditions for cross-country skiing.
He geared up and set out through the forest behind the century-old farmhouse where he lives with his wife, Susan, near East Grand Lake. Their 27-hectare homestead has been in the family since the 1870s.
About a kilometre out, Mr. O’Connor stopped for a rest. He was distinctly unwell. He had searing chest pain, was sweating copiously, and had increasing numbness in his legs.
“As time passed and the symptoms increased, I knew I had to get home,” he says. He got his skis back on and used his arms and poles to power a slow return home.
“It was the hardest physical thing I’ve ever had to do in my life,” he says.
Along the way, he had an epiphany: “I thought I was dying,” he says. “I had one objective in mind: to see my wife again.”
Susan O’Connor was out front shovelling when her husband hauled himself through the back door and into the kitchen, collapsing on the cot next to the wood stove. When she came in, her surprise at seeing him back so soon turned to concern.
She leapt into action, calling 911. It was 4:30 p.m.
Her husband was rushed by ambulance to the Upper River Valley Hospital in Waterville, where he was admitted to the emergency department before being transferred to the Saint John Regional Hospital’s Surgical Intensive Care Unit.
At the New Brunswick Heart Centre, he underwent a thoracic endovascular aortic repair, or TEVAR, to fix a tear in the inner layer of his main artery — the aorta.
This emergency was completely unexpected. At 75, Mr. O’Connor was active, had no history of cardiovascular disease and took no medications. A blood pressure issue he says he didn’t take seriously enough was the main risk factor for his condition.
Today, his blood pressure is controlled, and his CT scans look good. He’s replaced a daily cigar and drink with early-morning walks and yoga. His wife nourishes him with healthy homemade food and has bought a walkie-talkie for him to bring when he’s out in the woods.
Most of all, he has a new-found sense of being a survivor.
“I have an appreciation of everything that is like a rebirth,” Mr. O’Connor says. His gratitude is mixed with the realization of just how quickly your life can change.
"That morning, we thought we’d have the whole day. And then, you have a tragedy in the afternoon. Each day is very precious."
- Tom O'Connor, grateful patient
After he’d recovered, he wrote a letter to the hospital to express his gratitude.
Along with his letter, he included a cheque to give back to the system that was there for him in his time of greatest need. He wanted to pay forward the gift of life to the next patient.
Like Mr. Thornback, he says he is the beneficiary of a comprehensive cardiac care system, starting with the ambulance to the local hospital, the transfer to the Saint John Regional Hospital and his treatment at the Heart Centre.
“Many skilled people, only some of whom I met in person, contributed to my treatment,” he wrote in his letter. “I was thinking about these wonderful people. How can I give them a tiny fraction of what they gave me?”
People like Tom and Susan O’Connor have helped fund a number of groundbreaking investments at the New Brunswick Heart Centre so it can stay on the cutting edge of care.

In 2010, the Heart Centre achieved a first in Atlantic Canada when it pioneered the use of minimally invasive cardiac surgery, which uses smaller, less invasive incisions than conventional surgery.
Since the founding procedure – a mitral valve replacement – thousands of patients, including Mr. Thornback and Mr. O’Connor, have had minimally invasive surgeries for a range of procedures, including valve replacement and repair, coronary artery bypass grafting, cardiac tumour resections and congenital heart defect repairs.
The benefits are clear: smaller incisions have less post-operative bleeding, scarring and pain; fewer surgical wound complications such as infection and poor healing; a shorter recovery time and quicker return to work and daily living.
Along with the latest technology and tools, that innovation agenda extends to new processes and strategies to maximize their impact on the greatest number of patients.
“We always try to look for new ways of doing things that are more efficient, less costly, and better for patients,” Dr. Légaré says. “And that involves innovation on every level.”
He points to their Transcatheter Valve Implantation – or TAVI – Program, the first in Atlantic Canada. In the past, patients underwent open-heart surgery to replace or repair their aortic valves. A single procedure can take the surgeon all day. Patients are sedated, and some must go to the intensive care unit. This approach is still in use at some heart centres in Canada.
Compare that with the Heart Centre’s team-based TAVI Program, which includes members from clinical cardiology, interventional cardiology, cardiac surgery, cardiac anesthesia and interventional radiology. Using minimally invasive techniques, patients are awake during the procedure, and it takes a fraction of the time. And instead of a multi-day hospital stay, they are often discharged the next day, with excellent outcomes.
“It’s evolved dramatically,” he says. “We’re a program that constantly tries to understand how we can apply these technologies to a larger number of patients.”
Today, approximately 15 per cent of surgery patients undergo minimally invasive surgeries.
“But we still are stuck doing surgery with big, long instruments through small holes,” Dr. Légaré says.
Now, just over a decade after founding its minimally invasive program, the Heart Centre is welcoming the next generation of surgical technology into its operating rooms.
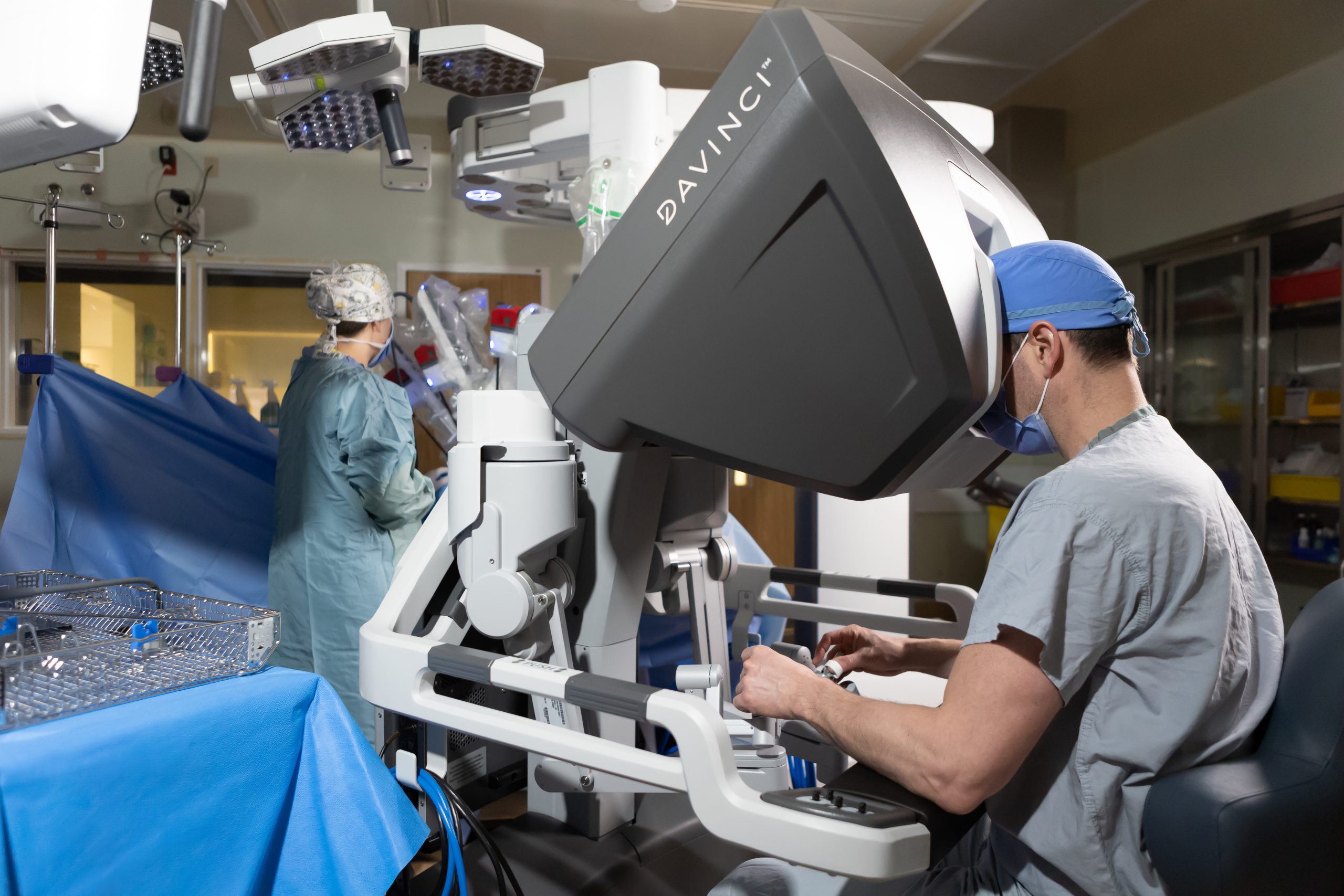
In October, the Saint John Regional Hospital Foundation’s ambitious campaign to acquire a da Vinci, the world’s leading surgical robot, reached its goal early, with more than 1,000 donors collectively donating more than $1.7 million by October.
The Thornbacks were among those donors. They’d been intrigued by the technology, which appealed to their interest in innovation. They gave $15,000 to the campaign.
“It just looked really interesting, and we are very supportive of New Brunswick health care modernizing,” Mrs. Thornback says.
The couple had moved from Ontario to New Brunswick in 2020 largely because of the province’s widespread fibre optic network, which allows them to run their tech company from here. They have been impressed in general by New Brunswick’s technology infrastructure and, specifically, the innovation agenda at Saint John Regional Hospital.
“They’re thinking of new ways to solve problems,” she says. “For a small province, they are really embracing technology.”
They had donated to the campaign before Mr. Thornback’s heart attack. During his treatment at the Heart Centre, surrounded by high-tech medical tools, he reflected upon how he was the beneficiary of previous investments in leading-edge equipment.
Several departments at the hospital will use the da Vinci, including Urology, Neurology, and the Heart Centre. That kind of cross-departmental collaboration and sharing is unique.
“It’s not just the cardiac surgery robot,” Dr. Légaré says. “It’s a robotic surgery program for the province on multiple levels.”
At the Heart Centre itself, he says there are many ways to use the robot beyond entirely robotic cardiac surgery, such as for bypass. Some 60 per cent of its surgeries involve bypass, which involves taking arteries from the leg or chest to create new routes to bypass blocked arteries. But some of those arteries are hard to access.
“A robot allows you to get at it much easier,” he says. “So you could do part of the procedure with the robot and the rest of the procedure normally.”
The Heart Centre is developing da Vinci training for its surgeons.
Meanwhile, as Dr. Légaré and his colleagues look to attract the next generation of specialists – many of whom studied robotic surgery as part of their medical training – the da Vinci is a powerful recruitment tool.
He is excited to welcome new colleagues to the Heart Centre who share a drive to build the program and bring new knowledge, energy and ideas.
“The practice is changing,” Dr. Légaré says. “We want to be a model for the future of cardiovascular care.”